Dr Simon Duffy warned a decade ago that the design of the national disability insurance scheme created perverse incentives, leaving it flawed from day one.
The British social policy reformer who warned a decade ago that the design of Australia’s national disability insurance scheme was flawed from the start and would be expensive and unsustainable said his worst fears have come true.
Dr Simon Duffy cautioned in 2013 that the “problems created by the current design are so great that it will force the federal government to redesign the system in a matter of just a few years”.
“I see no evidence that this is a sustainable solution, and the last 10 years rather prove the point to me,” Duffy told The Australian Financial Review last week.
Dr Simon Duffy, director of the UK Citizen Network Research at his home in Sheffield, UK on February 3. Denice Hough
Duffy, who has studied “entitlement” schemes for more than 20 years, warns that the design created perverse incentives that would blow out the scheme costs.
He also predicted the state governments and local providers would pull out – just as he had seen in other countries – leaving the national scheme the only place to get disability support.
“The question of what people need is very, very slippery,” he said.
“If, as a matter of public policy, you create systems that encourage the commodification of need or the creation of need out of difference, then you’re going to have a big headache.”
A decade ago, Duffy, like many, was genuinely excited about the promise of a well-funded, world-leading disability scheme that finally created meaningful rights for the previously neglected disabled community.
But after a study trip to Australia, Duffy expressed deep concern about the scheme’s development.
“The proposed design for NDIS seems to share many of the features of the worst systems and just a few of the features of the best systems,” Duffy wrote back then.
“It is clear that if you design a system in the wrong way, you can invite new levels of demand, generate inflationary expectations and increase costs in ways that seem totally detached from the real level of need in the community. Often, this money goes into services – but does not benefit people.”
He warned the “hyper-centralised” scheme “imposed an unnecessary, expensive and centralised bureaucratic infrastructure” that risked critical community and state-level services being withdrawn.
Duffy accurately predicted that an increasing number of complex, opaque, and constantly changing administrative rules would be needed to control costs. This would lead to endemic confusion and distrust.
“The problems created by the current design are so great that it will force the federal government to redesign the system in a matter of just a few years.”
Duffy returned to Australia last year to co-write another review with NDIS participant Dr Mark Brown for the Disability Advocacy Network Australia. They concluded the system design is “flawed” and “seems unsustainable”.
Dr Mark Brown with Dr Simon Duffy in August last year. Joe Armao
In Duffy’s mind, no particular group is to blame. “Cost pressures keep increasing as everyone tries to do their best to meet their needs. It is the design of the system, not the behaviour of any particular group, that is causing the current set of interconnected problems.”
This has created what is known as the tragedy of the commons – when individual behaviour works against what is in everyone’s best long-term interest.
A 14-month review confirmed Duffy’s worst fears about the sustainability of the scheme, agreeing with him that “a human right which cannot be sustained is a human right denied”.
A $1.4trn monster unleashed
Modelled on no-fault traffic accident schemes, the path-breaking disability insurance scheme was originally predicted to cost $13.6 billion a year in 2011.
Around 460,000 participants were predicted to join the scheme. This compared with around the 200,000 people who accessed a hotchpotch of community, state and federal services, costing around $9 billion at the time.
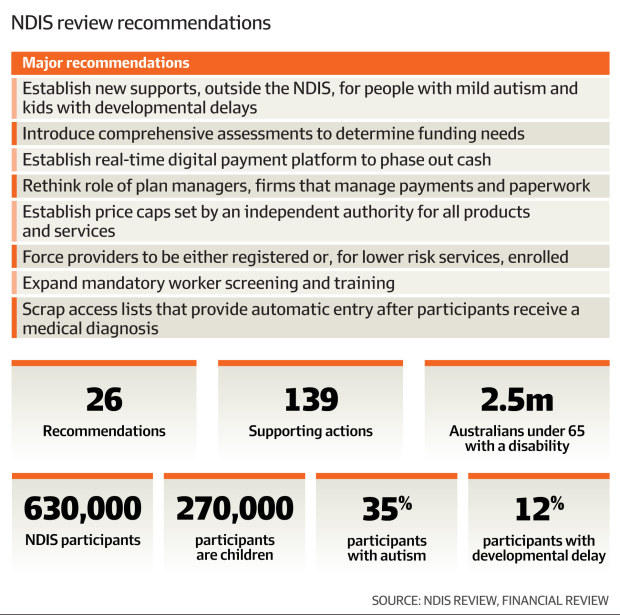
Despite not yet reaching maturity, the NDIS is supporting more than 610,000 people and is on track to cost $42 billion this financial year.
The government’s chief actuary, Guy Thorburn, peer-reviewed the latest sustainability report in October last year. Thorburn noted every projection had underestimated the cost of the scheme and said that instead of a predicted flattening, the number of child entrants had grown 22 per cent over the 2022-23 period.
The latest NDIS baseline projection is for the scheme to double in size to 1.2 million users at an annual cost of nearly $125 billion by 2034. That would mean the scheme is close to 3 per cent of GDP, double its current relative size.
Adjusting for last year’s $500 million of budget initiatives to manage the scheme better, the NDIS is still projected to cost $105 billion annually in a decade – well above the $95 billion target the budget and national cabinet projected for the scheme for 2034.
Thorburn’s analysis did not include the further $5 billion in savings the official review is projecting will occur by building community-based alternatives for the NDIS and better assessments. In any case, these $10 billion of reforms are effectively being paid for by federal GST guarantees, meaning the taxpayer will be on the hook regardless.
As of June 2022, the NDIA predicted the scheme’s lifetime cost to be $1.4 trillion, with an average gross lifetime cost of $2.6 million per participant. If Thorburn is correct that the reform savings will likely be washed aside by burgeoning child entrants, these eye-watering costs will be even higher.
Illusory results
Many of Australia’s most needy have materially benefited from the scheme’s support, and no one wants to return to the fragmented, poorly designed federal system of support that existed before the NDIS.
However, the official review was brutally honest in finding that the scheme’s key objectives were still far from being met.
For disabled people, health outcomes are nine times worse, school dropout rates are double, and employment levels are around two-thirds of persons without a disability.
A report by leading actuaries Taylor Fry and the Centre for International Economics looked hard to find and quantify benefits but could only identify around $7.6 billion in current benefits, mostly “life satisfaction”. But with the promise of more concrete benefits as early intervention begins to be effective.
However, with the scheme’s illusory outcomes, the review frankly admitted the mess the much-vaunted scheme is now in.
In perhaps its most damming finding, the review said the NDIS design encourages disabled people to present the “worst of themselves” to get, and retain, ongoing support. Precisely the opposite of the confident independent participants the scheme founders envisioned.
As Duffy warned, the financial incentive for providers who are paid for each service is to drive up activity rather than quality.
The review found that a scheme meant to give participants meaningful choice and control instead made them victims of complexity and uncertainty – all at a staggering cost.
As a senior official observed, the much-vaunted scheme has become “a monster”.
An ‘implementation’ problem
One of the reviewers, former NDIS chairman Bruce Bonyhady, is in no doubt where the scheme went wrong.
“The reason we’ve ended up where we are was because there were no supports outside the scheme,” said Bonyhady, who was the inaugural chairman of the NDIS.
“I think it largely was an implementation problem; it was never expected that all governments – and all governments did it – would vacate the field outside the NDIS. And then the moment that happened, of course, you’ve got these enormous pressures on the scheme.”
“A key part of our recommendations is you’ve got to structure and manage the entire ecosystem, and you can’t just focus on one mission, which is individualised support for people with the most significant disabilities.”
Former NDIS chairman Bruce Bonyhady, is in no doubt where the scheme went wrong.
The “oasis in the desert” problem was worsened by the NDIA’s lack of resources to manage the scheme properly and a lack of clear cost accountabilities. Under flawed agreements, the states had little responsibility or skin in the game for funding any cost overruns.
For Bonyhady, the answer is about restoring balance to the disability system. The states were always formally responsible for early childhood development and educational and other out-of-home supports for children.
Nowhere is the “oasis in the desert” problem more acute than with children with autism or delayed development.
Children with developmental delay were not even counted in the original 2011 Productivity Commission estimates, which focussed on permanent disability.
Disability groups successfully argued many conditions could be reversed if early intervention for developmental delay was funded, saving the NDIS higher costs in later life. Clinicians and researchers say the evidence is now even more apparent that early diagnosis and intervention dramatically improve the chances of turning around developmental delay and autism.
But the cost of this well-intentioned, but arguably naive, extension of the scheme was never properly calculated nor understood. And now risks the sustainability of the scheme for the other 500,000 permanently and seriously disabled people.
New entrants with developmental delay and autism account for 70 per cent of total new entrants, the only disability type that has been growing significantly above multiple forecasts.
All other disability types broadly reflect what was initially predicted, except delayed development and autism.
Autism advocate and retired data analyst Bob Buckley said disability officials have never been able to come to grips with delayed development and autism. Or the difference between prevalence and diagnosis.
“When the NDIS started, the actuaries told them that they should expect 9 per cent of participants to be autistic. But it’s now 35 per cent. The autism sector told them at the outset that they had the numbers very wrong.”
Misstep opens the autism ‘floodgates’
Buckley argues that the lack of clinical clarity around the definition of delayed development has opened a Pandora’s Box of claims.
“Developmental delay was introduced in section nine, the definition section of the NDIS Act.”
“It’s not a clinical definition. It’s not in the World Health Organisation [disease classification]. It’s not in the ICD 10 [International Classification of Diseases 10th Revision] nor in the DSM-5 [the Diagnostic and Statistical Manual of Mental Disorders].”
“It was created for the NDIS Act,” Buckley said.
Other autism advocates agree this was a crucial misstep.
“With the benefit of 20/20 hindsight, you can come back now and say, well, that just opened the floodgates to literally any kid who had a little bit of a problem, and that is where we’ve got ourselves in a lot of trouble,” the founder of the Sydney-based Autism Awareness Australia group, Nicole Rogerson said.
Autism Awareness Australia founder Nicole Rogerson says slightly quirky kids have “landed in the NDIS, which is a problem”. Lee Besford
“We now have these ridiculous inflated numbers of children in the scheme that have a diagnosis of autism, but who probably just are not. They need some kind of help, they’re slower at learning, they’re slightly quirky kids, but they’ve all landed in the NDIS, which is a problem.”
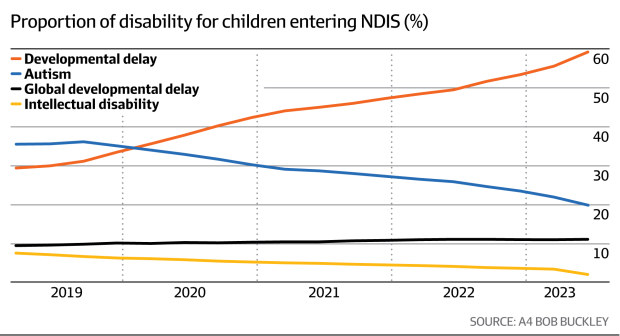
Buckley is a retired data analyst and said it is delayed development and not autism that is driving the rapid increase in young children entering the NDIS. He points to data showing autism has almost halved as a proportion of young children entering the NDIS over the last four years. The proportion of developmental delay has doubled in the same period.
Developmental delay often presents as autism in older children and an earlier Taylor Fry report noted scheme exits are a third of what was expected.
This points to a fundamental failure of what is meant to be an early intervention model and to the lurking time bomb in the NDIS costs.
Officials now fear many of the older children with autism currently in the scheme will remain participants in their adult lives, dramatically lifting costs across the 2030 and 2040s.
Noting that one in five children have developmental issues, the review called for a “mainstream” solution. The national cabinet has accepted the need for a significant structural response. Ten billion dollars over 10 years is to be used to gear up a set of foundation supports, offering community alternatives for not just autism, but also other less severe disabilities better treated outside the NDIS.
This foundational policy work, together with the better administration of the scheme and improved assessments and plans, is now being heavily relied on to reduce the baseline assumption that the scheme will double by 2034.
The massive cost of the scheme comes as pressures to better fund a raft of social services, from aged care to mental health, puts enormous stress on a personal tax system that now accounts for 50 per cent of government revenues.
But whatever the NDIS fiscal challenges, polling reveals the scheme is strongly supported across the community. This, in part, reflects the pervasiveness of various disabilities across the nation. And that for many disabled people, the NDIS is their only lifeboat. Full stop.
Like Medicare, the NDIS already has a special spot in the community. Being seen to be pulling back on support would be political dynamite, meaning the scheme, in whatever form, is here to stay.